Mr Ponosh and Ponosh Vascular provides a comprehensive diagnostic and treatment management solution to all vascular disorders.
Utilizing up to date and cutting edge, evidence based management, Mr Ponosh will tailor your treatment for the very best outcome through conservative medical therapies, minimally invasive endovascular (keyhole) treatments or open surgical operations.
Please see below for information sheets relating to some some commonly managed conditions.
Ponosh Vascular provides the very latest, up to date and comprehensive diagnostic and management service of all vascular conditions. Utilizing the optimal conservative medical therapies, minimally invasive endovascular techniques and contemporary surgical options, we specialise in:
Peripheral Arterial Disease (PAD) is a condition where the arteries become narrowed or blocked by fatty deposits called atherosclerosis, more commonly known as “hardening of the arteries”.
Whilst this can occur in many arteries in you body, significant problems may arise when this narrowing occurs in the arteries of your leg.
Over the years cholesterol and calcium build up inside the arteries causing the narrowings. This occurs much earlier in people who have these risk factors
PAD occurs as a range of disease progressing from simple narrowings without many symptoms to conditions that pose increased threats to your legs.
People with any of these conditions need management of all their risk factors as underlying PAD suggests a higher risk of stroke or heart attack.
If you have any of the above symptoms or are concerned that you do, please see your General Practitioner in the first instance. They may be able to clarify other possible diagnoses but if they are concerned they will refer you to a Vascular & Endovascular Surgeon, such as Mr Ponosh.
Whilst walking pain or claudication may limit your lifestyle, it may not require an urgent referral, however if you have rest pain or a non-healing ulcer, an urgent review is essential.
Your GP may contact Mr Ponosh’s office directly, however in some cases they will provide you a referral to contact the office yourself. Mr Ponosh’s caring and helpful staff will walk you through the process of making an appointment with Mr Ponosh. His staff may also contact you directly. For further information please regarding referrals, please go to Make an Appointment.
When you see Mr Ponosh, he will undertake a full history and appropriate examination. In many instances (if required) he will order appropriate tests before he sees you to streamline your management and avoid unnecessary appointments. These tests are bulk-billed at all times if possible. These tests may include ultrasounds, CT scans or blood tests. In some cases, additional tests and appointments may be required.
Based upon Mr Ponosh’s expert specialized review, an appropriate treatment plan will be suggested and explained to you in an open, straight-forward, jargon-free manner with all options and questions addressed.
In many cases, aggressive treatment is not required. In many patients, where there is a minimal lifestyle impact or minimal symtoms, no treatment beyond treating the underlying risk factors that cause the PAD is needed.
In mild symptoms, an active exercise program and risk factor treatment has been shown to have some benefits in improving outcomes especially in those with claudication. Mr Ponosh will discuss this with you if appropriate.
However treatment is appropriate if you develop :
Treatment is different for every patient and depends on multiple factors including; underlying symptoms, nature of your disease, your age and underlying health issues, medications and expected outcomes for you. Mr Ponosh takes all these factors as well as his vast personal experience and evidence-based practice to tailor the most optimal treatment for you at the lowest risk and with the best outcome. Your treatment may include one or a combination of the below options.
Conservative
This means a “watch and wait” approach. As described above, if your PAD is only mild, treatment is not always in your best interests and may not always have the best outcome for you. In these cases, Mr Ponosh in conjunction with your GP and occasionally other specialists such as diabetic or heart specialists (if required) will manage you risk factors improving your long term outcomes.
Other options such as a walking program may also be discussed with you.
Beyond the medications used to treat your risk factors and some blood thinners like aspirin, there are no other medications shown to make a “real-life” difference in your PAD.
Mr Ponosh may suggest regular review (often annually) to keep a close eye on your PAD. Of course is you develop any concern’s or worsening symptoms, please contact Mr Ponosh’s office.
Endovascular or Angiographic Treatments
Endovascular or “key hole” angiogram treatments are minimally invasive procedures that usually require a day-stay or a short overnight stay. They are undertaken with an anaesthetist usually done under a local anaesthetic with sedation providing a “twilight” anaesthetic. Endovascular procedures are undertaken through a small needle access through your groin directly into your arteries. They are low risk, essentially pain-free procedures which utilize state of the art modern technologies for excellent outcomes. The results are almost immediate and have a very rapid return to your normal lifestyle.
These procedures allow Mr Ponosh to undertake a diagnostic angiogram to further assess your PAD, and in most cases, proceed to the below procedures during the angiogram to treat and cure your disease :
Please follow the link to further information on Angioplasty & Stenting.
Open Surgical Techniques
These are more invasive procedures done through larger open incisions, often under a general or spinal anaesthetic.
Open surgical options may be utilized for more complicated or extensive disease or in some cases where it has been shown to provide the best outcome.
These procedures whilst shown to be safe and durable have different and often higher risks than endovascular treatments and are thus only used when appropriate. These procedures may include a bypass operation in which your own vein or a plastic tube is used to bypass the blockage in your artery or a endarterectomy where a more localized blockage is surgically removed.
These procedures often need a 1 night intensive care stay with a 5-7 day stay in hospital. Mr Ponosh would discuss these procedure with you at length.
An angiogram is a procedure to visualize the flow through your arteries. Whilst Mr Ponosh will organize ultrasounds, CT or MRI scans to assess and diagnose your vascular disease, an angiogram may be required for further information or to ultimately treat your arterial disease. In some cases, these procedures can also ve used to treat your veins (venogram).
Endovascular or “key hole” angiogram treatments are minimally invasive procedures that usually require a day-stay or a short overnight stay. They are undertaken with an anaesthetist usually done under a local anaesthetic with sedation providing a “twilight” anaesthetic.
Endovascular procedures are undertaken through a small needle access through your groin directly into your arteries. Dye is injected through the needle or access tube (sheath) to show the flow through your arteries and is shown by x-rays taken during the procedure to confirm the narrowing’s or other disease that needs to be treated. The procedure takes between 45-60 minutes in most cases.
They are low risk, essentially pain-free procedures which utilize state of the art modern technologies for excellent outcomes. The results are almost immediate and have a very rapid return to your normal lifestyle.
The procedure will have been discussed at length with Mr Ponosh in his office. Mr Ponosh will the procedure to you in an open, straight-forward, jargon-free manner with all options and questions addressed. The benefits and the risks will also be discussed. A consent or permission form will be signed by you and Mr Ponosh.
You will be admitted to the hospital for a few hours in advance of your procedure to prepare for the angiogram. Mr Ponosh’s staff will confirm these times in writing with you and provide clear information on eating, drinking and fasting times. Advice will also be provided by Mr Ponosh and his staff regarding your medications. This will particularly apply to any blood thinners or diabetic medications. Please advise us if you are taking >>>>>>>>>>>>>>>. The anaesthetist will usually contact you in the days before your procedure for further information.
During this preparation time in hospital, if you have any worries or queries do not be afraid to ask. It is necessary to put on a hospital gown and usually the hair at the groin area needs to be trimmed before the angiogram. The procedure will take place in area known as an Angiography Suite. This is like an operating theatre however it is specialized for angiograms and has additional equipment including the special x-ray machines.
The anaesthetist will place a small drip in your hand or arm and start your “twilight” anaesthetic. You will be positioned on the procedure table and your groin skin will be cleaned to prevent infection. The cleaning preparation is often a little cole. You will be then covered with sterile drapes. Occasionally your face will be covered but a “tent” will be made to make you feel comfortable. You will be asked to lay as still as possible however if any concerns or questions arise, the nursing and anaesthetic staff will assist you. You may feel some pushing and pressure in your groin, however the procedure should be as discomfort-free as possible.
The doctor will inject a local anaesthetic into the skin at the groin numbing the area. Then the fine tube (sheath) is inserted into the vessel. With the help of wires other small long tubes called catheters can be maneuvered through the blood vessels and positioned as desired. X-ray pictures are taken whilst dye is injected down the catheter into the blood vessels. The dye may cause a hot flush and the feeling of having to pass urine. Both will subside after a few seconds. Multiple injections are necessary to see the full length of the blood vessel and the x-ray machine or the table will be moved in-between them. Mr Ponosh will identify the diseased arteries and treat your disease using either :
Some narrowed arteries (and rarely veins) are treated by passing a balloon across the diseased segment and then inflating it. The balloon will dilate the narrowing treating the blockage and improving your symptoms. The balloon is then removed. Mr Ponosh may elect to use new state of the art “drug coated” angioplasty balloons in some cases which coat the treated artery with a special drug. These special balloons have been shown to have very good long term outcomes especially in cases of re-narrowing.
In some cases Mr Ponosh may decide a stent is the best option to treat your narrowed arteries (or vein). Stents are either a bare metal scaffold or a plastic covered metal scaffold to help hold the artery open. The use of these stents are based upon Mr Ponosh’s vast personal experience and evidence based medicine to provide you the optimal outcome. These are minimally invasive devices which are permanent and often have special drugs coating them to help improve outcomes.
They may be used to treat narrowing or some cases aneurysm’s (blow outs or dilations) of your arteries.
This is a key-hole device used in conjunction with ballooning or stenting to “drill” or excise out arterial disease. It is used in specific cases to improve outcomes.
This is a procedure usually used on veins and occasionally arteries in which small metal coils and permanently placed in vessels to block them off. This is often used on “leaky” veins such as an ovarian vein and may be part of varicose vein treatment. The coils are made from platinum and will not cause issues with other x-rays or airport metal detectors. Mr Ponosh will discuss there use with you if required.
When the procedure is completed all access sheaths are removed from you. A special staple or plug device may be used to the small hole in your artery. Pressure will be applied to the groin for up to fifteen minutes and a small pressure device (Fem-Stop) may be placed on your groin for an hour or so. You will awaken from your twilight anaesthetic and moved to the recovery area where nurses will be keeping a close eye on you. Approximately 2-4 hours of bed rest are necessary to prevent any bleeding from the puncture site. The nursing staff will check the groin, and foot pulses at regular intervals.
Your usual medication may be adjusted after this procedure however this will be clearly detailed to you. Mr Ponosh will speak to you after your procedure and you will discuss any queries or questions with you.
You will either stay overnight or be discharged later in the day if a day case was planned. Nursing staff will keep you well looked after during your stay. Mr Ponosh’s staff will be in contact with you in the days following your procedure to arrange your follow-up in his office and any ultrasounds if required.
Please see Mr Ponosh’s angiogram discharge information sheet for discharge advice.
An angiogram/ angioplasty is a very safe low risk procedure. Mr Ponosh has decided and discussed with you that although there are risks inherent to every procedure, the benefits to you dramatically outweigh them and the angiogram is the best treatment for you. If you have any concerns please contact your GP, your hospital or Mr Ponosh’s rooms directly.
Bleeding
As the operation is performed on blood vessels a small amount of bleeding can sometimes occurs. This is often easily treated with some pressure but it is common to have some bruising to the area after the procedure. You may also develop a small lump which will resolve by itself. Serious bleeding is very uncommon.
False aneurysm
Very rarely a lump may occur which is in flow with the artery. This is because of some continued bleeding from the puncture site. This is called a pseudoaneurysm. This pseudoaneurysm may settle by themselves whilst other may require an additional procedure to fix them. Mr Ponosh will see you in regards to this.
Pain/Discomfort
Main and discomfort is usually minimal during the procedure and after. Occasionally you can get some bruising and discomfort to the groin in the following days but this is minor. If you are concerned or the pain is significant please seek advise.
Allergic reactions to the dye
Very rare
Damage to blood vessels
Usually these problems can be dealt with at the time of the procedure, but in rare instances open surgery is necessary.
Equipment failure
It is theoretically possible for a catheter, wire or device to break and leave a fragment inside the body. This is extremely rare.
Failure of technique
Occasionally it is not possible to perform the angioplasty or the procedure does not show the desired result. In very rare circumstances a failed procedure can actually make the blood flow worse.
Kidney damage
The dye used is excreted via the kidneys, which in most patients is completely normal. However, especially in patients poor kidney function, the dye can lead to deterioration in kidney function. Angiograms are used in patients with kidney disease often and safely but additional precautions are required such as admission the night before the procedure, additional fluids and modifying your medications. Mr Ponosh will discuss these with you. Patients on dialysis do not need additional precautions and angiograms are completely safe.
Varicose veins are abnormally dilated and tortuous veins, often visible just beneath the skin. They can vary in size from quite small (2-3mm across) to very large (2-3cms across). Very small veins are called “thread veins” or “spider veins”. These veins are different to varicose veins because they are situated much closer or within the overlying skin. Although they may be unsightly, they are mainly a cosmetic issue and are often more challenging to treat.
Varicose veins may simply be a cosmetic issue but they can cause a range of symptoms and problems.
Veins are blood vessels that drain used blood up the leg back to the heart. There are two types of veins in your legs. The deep veins which do the bulk of the work, and the more superficial draining system.
The deep veins are larger veins deeper in the muscles that drain the majority of your legs blood back to the heart. These veins develop conditions such as deep vein thrombosis, colloquially known as “economy class syndrome”
The skin draining system consists of 2 veins, the long saphenous running from the ankle to the groin on the inside of your leg and the short saphenous vein running up you calf from the Achilles to the back of your knee. These veins drain into the deep system. The malfunctioning of these veins are the common cause of varicose veins and are the focus of treatment in many cases.
These veins have no pump but rely on a system of hydraulics moving blood up the leg against gravity. When compressed, blood moves up these veins with one way valves stopping the blood flowing back down the leg. Under certain circumstances these valves fail or become “incompetent” with blood now flowing up and down the leg. This reverse flow back down the leg causes abnormally high pressure in the veins. The veins can not cope with this abnormally high pressure and dilate, thus causing varicose veins.
In addition, veins particularly at the ankle are “watertight” at these high pressures and thus become “leaky”, causing many more sinister, non just cosmetic symptoms such as swelling, pigmentation, itching and even ulcers.
Varicose veins are associated with :
Varicose veins can cause :
This is generally a personal decision for many patients particularly if you veins are purely a cosmetic concern. If they bother you, given the low risk, often minimally invasive and durable solutions now available for treating varicose veins, in most instances Mr Ponosh would recommend having them treated.
Veins will never improve if left alone and will only progress, so treating them in most cases makes sense.
However if you have more complicated veins (symptoms 5-10 from above) treatment of your veins is essential to avoid more sinister outcomes.
Your GP may contact Mr Ponosh’s office directly, however in some cases they will provide you a referral to contact the office yourself. Mr Ponosh’s caring and helpful staff will walk you through the process of making an appointment with Mr Ponosh. His staff may also contact you directly. For further information please regarding referrals, please go to Making an Appointment.
When you see Mr Ponosh, he will undertake a full history and appropriate examination. In many instances (if required) he will order appropriate tests before he sees you to streamline your management and avoid unnecessary appointments. These tests are bulk-billed at all times if possible. These tests most commonly include an ultrasound of your legs and occasionally your abdomen. In some cases, additional tests and appointments may be required.
Based upon Mr Ponosh’s expert specialized review, an appropriate treatment plan will be suggested and explained to you in an open, straight-forward, jargon-free manner with all options and questions addressed.
Treatment is not “one size fits all” especially when it comes to varicose veins.
Mr Ponosh if one of the few vascular specialists in Perth to provide a true comprehensive management service for veins offering all the up-to-date available therapies to tailor your treatment for the best outcome. His experience of treating veins extends into the thousands over many years.
Our service is not a matter of “square peg for a round hole” like others do but finding the correct round peg for that round hole.
Options are different for every patient and depends on multiple factors including; underlying symptoms, nature of your disease, your age and underlying health issues, medications and expected outcomes for you. Mr Ponosh takes all these factors as well as his vast personal experience and evidence-based practice to tailor the most optimal treatment for you at the lowest risk and with the best outcome.
Your treatment may include one or a combination of the below options :
These include wearing compression stockings, elevation, and exercise.
A more modern and minimally invasive method of treating the source of the varicose veins in a “walk in walk out” room based treatment. It is conducted under local anaesthetic with excellent long term outcomes.
Click to see additional information sheet
This is a similar to RFA however used laser rather than radiofrequency energy. Very similar outcomes.
Click to see additional information sheet
This is used in all types of varicose veins and a microinjection technique may be used for thread veins. It is a simple low risk minimally invasive solution for many veins
It may not be as effective as other techniques for larger varicose veins especially if there is a major draining vein malfunction.
Click to see additional information sheet
This is still a common form of treatment for varicose veins and is a an effective way of removing veins. Techniques have changed over the years with excellent outcomes and shortened recovery.
Content coming soon…
An artery is a blood vessel that carries oxygen-rich blood from your heart to all the parts of the body. An aneurysm is a condition where the walls of the artery dilate or “balloon” out. This ballooning may increase in size and finally burst leading to bleeding or the artery blocking off. Aneurysms can be of different types depending on its location:
Thoracic aortic aneurysm: Aneurysm in the aorta (major artery arising from the heart) that runs down your chest
Abdominal aortic aneurysm: Aneurysm in the aorta that extends to your abdominal region
Peripheral aortic aneurysm: Aneurysm in arteries found in the peripheral regions such as popliteal artery (which runs down the back of your lower knee and thigh), femoral artery (groin area).
Most aneurysms are caused by degeneration or the process of aging on the wall of the artery. The strength of arteries is associated with collagen and elastin, the same structures that give our skin elasticity. As time goes on, these structures degenerate or breakdown causing weakness of the artery that can cause the ballooning of the artery. In some cases they can be caused by inflammation, leading to the weakening or breakdown of the artery walls. This inflammation can result from atherosclerosis, which is characterized by the deposition of plaque (calcium, cholesterol and minerals). The plaque deposits weaken the inner wall of the artery, making it more susceptible to swelling and rupture.
In some rare instances diseases like Marfan’s syndrome (genetic disorder that affects the tissues holding the body’s cells, tissues and organs together) can cause aneurysms as well as trauma or a variety of much rarer causes.
The commonest group susceptible to aneurysms are males over the ages of 60 with a history of smoking. A family history may occasionally be involved.
The majority of aneurysms may not show any symptoms. However, when symptoms do appear, they generally depend on the region of the aneurysm.
Symptoms for a thoracic aortic aneurysm may rarely include:
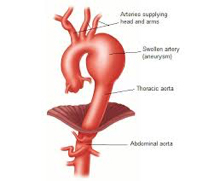 These are aneurysms of the aorta within your chest.
These are aneurysms of the aorta within your chest.
TAA’s are a progressive dilation of the aorta. Most aneurysms start and stay small. The normal male aorta measures 15-17mm and in some cases over time will progressively dilate. They are of concern when they approach 60mm or demonstrate more rapid patterns of growth in many instances.
Most aneurysms are found by accident, usually during the investigation of other complaints.
The cause of aneurysm is not well known, but there are numerous risk factors that include:
If you are known to have, or if you are likely to develop an aneurysm disease, it is recommended that you optimise your lifestyle by:
In most cases, small aneurysms are completely safe and should not worry you. They also have minimal or no symptoms. These stable or slowly growing aneurysms simply need a regular check up with a ultrasound or CT scan with your vascular surgeon to ensure they remain safe.
Treatment may never be needed but if it does require treatment these close surveillance allows safe and effective treatment at the right time avoiding the severe complications that aneurysms can occasionally pose.
As they grow often over a period of years, the walls may thin as the aneurysm balloons to a point that the aneurysm may leak or rupture. This in most cases is associated with aneurysms in excess of 60mm. This is a life-threatening complications and is associated with severe internal bleeding and clots. More easily manageable, or smaller aneurysms simply need lifestyle changes, a watchful eye and regular checkups with your vascular surgeon.
Most aneurysms are found by accident during other tests. Your GP may then send you to see Mr Ponosh directly.
If you think you are at risk of having an aneurysm OR have a family history of aneurysm you should:
See your GP: Your GP will assess you and may organize an ultrasound scan. If evidence presents of an AAA, your GP will almost always send you onto a Vascular Surgeon, such as Mr Ponosh.
If you know you have an TAA which is under surveillance or observation by Mr Ponosh (ie; it is asymptomatic and smaller than the treatment cut-off size), you would normally have a non-invasive ultrasound at a specialised vascular ultrasound practice on a regular basis and be observed every 6-12 months by Mr Ponosh.
If you TAA reaches a size of approximately 60mm or demonstrates a period of rapid growth, Mr Ponosh may suggest consideration for treatment. A CT scan is usually arranged at this time for more accurate assessment of your aneurysm and its anatomy.
Mr Ponosh will keep a very close eye on your AAA. When it reaches an appropriate size it may be considered for repair. This not only depends on the size of the AAA but also on the location, anatomy, your age and your general health.
If you have very complicated aneurysmal anatomy, especially if the aneurysm is very close to other main arteries (arm, brain or bowel), due to the increased complexity of the repair options and the risk this imposes, Mr Ponosh may suggest maintaining close observation until the AAA reaches a larger size. At this point the risk of repair is more appropriate to the risk of the aneurysm. Also if you general health is poor, Mr Ponosh may also suggest ongoing observation rather than repair due to the risks to your life and lifestyle.
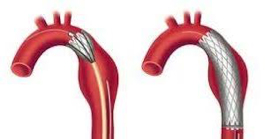
If repair of your TAA is recommended in the majority of cases Mr Ponosh will recommend an endovascular or “keyhole repair”. In most cases this is a very straight forward and uncomplicated procedure. This has been proven to be a very effective and durable repair using special “stents” to seal the aneurysm. In this procedure usually conducted under a general or spinal anaesthetic, Mr Ponosh makes a very small incision (5mm) in the groin region and guides a catheter (thin tube) through the blood vessel. He then uses live X-ray images to guide a stent-graft to the site of the aneurysm. The graft re-lines the aorta, sealing the aneurysm and prevents it from rupturing. It takes in most cases approximately 60 minutes. You may be required to stay in hospital for 2-3 days until recovery. In time, the aneurysm may even shrink because of the stent-graft.
In some cases a more complicated EVAR known as a Fenestrated Endovascular Repair (FEVAR) is undertaken. This is usually cases where the aneurysm is close to other important arteries. This requires a custom made, hand sown stent that seals above these important arteries. This custom made graft has small holes (fenestrations) which are carefully lined up with important arteries, through which additional stents are placed from the main graft to seal the aneurysm. This may take 3-4 hours in more complicated cases and is a riskier procedure.
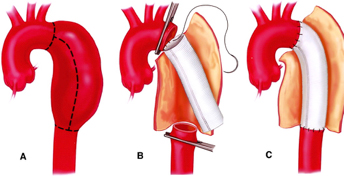
This is the traditional repair method for aneurysms. These repairs are rarely undertaken. They are usually reserved for cases that are not suitable for EVAR or FEVAR, are urgent and can not wait for custom made grafts, or occasionally in young patients.
It is a more involved procedure undertaken through a long cut in your chest in which a new plastic tube is hand stitched in place by Mr Ponosh. It takes several hours to complete, has a hospital stay of 10-14 days and several week to recover from.
Mr Ponosh will spend a lot of time discussing aneurysm repair and the risks with you in detail and in a easy to understand, reassuring manner. The risks of aneurysm treatment can include:
While the risks of treatment are large, the risk of not treating the aneurysm can be worse. Mr Ponosh will be able to provide you with the information you need to make an informed choice and be reassured and fully informed.
An artery is a blood vessel that carries oxygen-rich blood from your heart to all the parts of the body. An aneurysm is a condition where the walls of the artery dilate or “balloon” out. This ballooning may increase in size and finally burst leading to bleeding or the artery blocking off. Aneurysms can be of different types depending on its location:
Aneurysm in the aorta (major artery arising from the heart) that runs down your chest
Aneurysm in the aorta that extends to your abdominal region
Aneurysm in arteries found in the peripheral regions such as popliteal artery (which runs down the back of your lower knee and thigh), femoral artery (groin area).
Most aneurysms are caused by degeneration or the process of aging on the wall of the artery. The strength of arteries is associated with collagen and elastin, the same structures that give our skin elasticity. As time goes on, these structures degenerate or breakdown causing weakness of the artery that can cause the ballooning of the artery. In some cases they can be caused by inflammation, leading to the weakening or breakdown of the artery walls. This inflammation can result from atherosclerosis, which is characterized by the deposition of plaque (calcium, cholesterol and minerals). The plaque deposits weaken the inner wall of the artery, making it more susceptible to swelling and rupture.
In some rare instances diseases like Marfan’s syndrome (genetic disorder that affects the tissues holding the body’s cells, tissues and organs together) can cause aneurysms as well as trauma or a variety of much rarer causes.
The commonest group susceptible to aneurysms are males over the ages of 60 with a history of smoking. A family history may occasionally be involved.
The majority of aneurysms may not show any symptoms. However, when symptoms do appear, they generally depend on the region of the aneurysm.
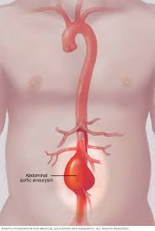 These are aneurysms of the aorta within your abdomen. They are the commonest form of aneurysm we see.
These are aneurysms of the aorta within your abdomen. They are the commonest form of aneurysm we see.
AAA’s are a progressive dilation of the aorta. Most aneurysms start and stay small. The normal male aorta measures 15-17mm and in some cases over time will progressively dilate. They are of concern when they approach 50mm or demonstrate more rapid patterns of growth in many instances.
Most aneurysms are found by accident, usually during the investigation of other complaints.
The cause of aneurysm is not well known, but there are numerous risk factors that include:
If you are known to have, or if you are likely to develop an aneurysmal disease, it is recommended that you optimise your lifestyle by:
In most cases, small aneurysms are completely safe and should not worry you. They also have minimal or no symptoms. These stable or slowly growing aneurysms simply need a regular check up with a ultrasound or CT scan with your vascular surgeon to ensure they remain safe.
Treatment may never be needed but if it does require treatment these close surveillance allows safe and effective treatment at the right time avoiding the severe complications that aneurysms can occasionally pose.
As they grow often over a period of years, the walls may thin as the aneurysm balloons to a point that the aneurysm may leak or rupture. This in most cases is associated with aneurysms in excess of 50mm. This is a life-threatening complications and is associated with severe internal bleeding and clots. More easily manageable, or smaller aneurysms simply need lifestyle changes, a watchful eye and regular checkups with your vascular surgeon.
Most aneurysms are found by accident during other tests. Your GP may then send you to see Mr Ponosh directly.
If you think you are at risk of having an aneurysm OR have a family history of aneurysm you should:
See your GP: Your GP will assess you and may organize an ultrasound scan. If evidence presents of an AAA, your GP will almost always send you onto a Vascular Surgeon, such as Mr Ponosh.
If you know you have an AAA which is under surveillance or observation by Mr Ponosh (ie; it is asymptomatic and smaller than the treatment cut-off size), you would normally have a non-invasive ultrasound at a specialised vascular ultrasound practice on a regular basis and be observed every 6-12 months by Mr Ponosh.
If you AAA reaches a size of approximately 50mm or demonstrates a period of rapid growth, Mr Ponosh may suggest consideration for treatment. A CT scan is usually arranged at this time for more accurate assessment of your aneurysm and its anatomy.
Mr Ponosh will keep a very close eye on your AAA. When it reaches an appropriate size it may be considered for repair. This not only depends on the size of the AAA but also on the location, anatomy, your age and your general health.
If you have very complicated aneurysmal anatomy, especially if the aneurysm is very close to other main arteries (kidney or bowel), due to the increased complexity of the repair options and the risk this imposes, Mr Ponosh may suggest maintaining close observation until the AAA reaches a larger size. At this point the risk of repair is more appropriate to the risk of the aneurysm. Also if you general health is poor, Mr Ponosh may also suggest ongoing observation rather than repair due to the risks to your life and lifestyle.
If repair of your AAA is recommended in the majority of cases Mr Ponosh will recommend an endovascular or “keyhole repair”. In most cases this is a very straight forward and uncomplicated procedure. This has been proven to be a very effective and durable repair using special “stents” to seal the aneurysm. In this procedure usually conducted under a general or spinal anaesthetic, Mr Ponosh makes a very small incision (5mm) in the groin region and guides a catheter (thin tube) through the blood vessel. He then uses live X-ray images to guide a stent-graft to the site of the aneurysm. The graft re-lines the aorta, sealing the aneurysm and prevents it from rupturing. It takes in most cases approximately 60 minutes. You may be required to stay in hospital for 2-3 days until recovery. In time, the aneurysm may even shrink because of the stent-graft.
In some cases a more complicated EVAR known as a Fenestrated Endovascular Repair (FEVAR) is undertaken. This is usually cases where the aneurysm is close to other important arteries such as kidney or bowel. This requires a custom made, hand sown stent that seals above these important arteries. This custom made graft has small holes (fenestrations) which are carefully lined up with important arteries, through which additional stents are placed from the main graft to seal the aneurysm. This may take 3-4 hours in more complicated cases and is a riskier procedure.
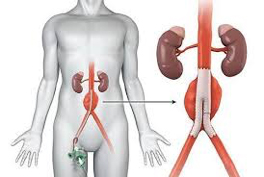
This is the traditional repair method for aneurysms. This type of repair is only undertaken in 5-10% cases. They are usually reserved for cases that are not suitable for EVAR or FEVAR, are urgent and can not wait for custom made grafts, or occasionally in young patients.
It is a more involved procedure undertaken through a long cut in your abdomen in which a new plastic tube is hand stitched in place by Mr Ponosh. It takes several hours to complete, has a hospital stay of 10-14 days and several week to recover from.
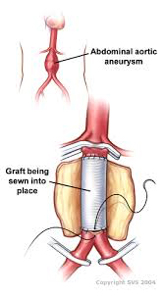
Mr Ponosh will spend a lot of time discussing aneurysm repair and the risks with you in detail and in a easy to understand, reassuring manner. The risks of aneurysm treatment can include:
While the risks of treatment are large, the risk of not treating the aneurysm can be worse. Mr Ponosh will be able to provide you with the information you need to make an informed choice and be reassured and fully informed.
Content coming soon…
Ulcers are unfortunately a not uncommon problem that Mr Ponosh sees. They also are a very serious problem.
Ulcers are wounds, commonly to legs, ankles at feet that occur spontaneously or more frequently after minor trauma such as a new pair of ill-fitting shoes.
They are deep wounds with areas of skin and tissue loss. They do not heal quickly or only deteriorate, persisting for weeks or more
There are many causes of ulcers that cause wounds to spontaneously occur or worsen a minor injury :
Ulcers can most commonly present as an area of skin and tissue loss. These may be small or in some cases which have been left untreated may be quite large. They can occur at areas of trauma such as the shin, or heel/toes after wearing ill fitting shoes. They can spontaneously occur over the ankles and on/in between your toes.
They may be painful, however in some cases especially if you are diabetic may be completely unnoticed and pain free. They may become infected with red, hot and swollen skin around them. Most concurringly, if they progress underlying bone and tendons can be exposed which is a very serious problem.
Ulcers can often be ignored and under appreciated by medical practitioners, however they should never be and always should be seen and managed by an expert such as Mr Ponosh. Most small ulcers are relatively straight-forward to fix but if they are large or complicated, they can take months to heel and are more challenging.
All ulcers with a known cause, presumed cause or risk factor or persisting for more than 2-3 weeks should be referred to a specialist wound service such a Mr Ponosh provides.
Mr Ponosh has a vast experience in managing ulcers and it is an area or particular interest. Mr Ponosh has a long history as a Senior Consultant to the Sir Charles Gairdner Foot & Leg Ulcer Clinic.
Ulcers in most people with underlying causes will never heal by themselves.
Left untreated, ulcers will often progress and place you at risk of severe infection or even blood poisoning (septicaemia). Chronic ulcers can cause you to feel chronic pain, feel chronically ill and tired and may get in the way of your quality of life.
Ulcers may stop you proceeding to other operations such as hip or knee replacements.
Most concerningly, as these ulcers progress and expose tendon or bone, these ulcers may put toes or even your foot at risk.
Your GP may contact Mr Ponosh’s office directly, however in some cases they will provide you a referral to contact the office yourself. Mr Ponosh’s caring and helpful staff will walk you through the process of making an appointment with Mr Ponosh. His staff may also contact you directly. For further information please regarding referrals, please go to Make an Appointment.
When you see Mr Ponosh, he will undertake a full history and appropriate examination. In many instances (if required) he will order appropriate tests before he sees you to streamline your management and avoid unnecessary appointments. These tests are bulk-billed at all times if possible. These tests may include ultrasounds, CT scans or blood tests. In some cases, additional tests and appointments may be required.
Based upon Mr Ponosh’s expert specialized review, an appropriate treatment plan will be suggested and explained to you in an open, straight-forward, jargon-free manner with all options and questions addressed.
They key to curing your ulcers is the diagnosis and treatment of underlying causes. Treating ulcers effectively also relies on a team approach which Mr Ponosh will supervise and co-ordinate. Mr Ponosh’s multidisciplinary ulcer team includes :
In most cases these treatments can be undertaken as a outpatient with Mr Ponosh managing you through his rooms but occasionally if more severe, Mr Ponosh may need to admit you to hospital for more appropriate treatment.
Treatment may include :
Some ulcers will be relatively simple to treat over a few weeks, however other ulcers may take many weeks or months to heal even with aggressive treatment.
Patience, persistence and compliance is the key to healing these wounds.
In almost all cases we do heal the ulcer although there is the rare instance of unusual ulcers that do not heal. This is very rare.
Ulcers, especially in damaged skin such as venous ulcers do have a tendency to recurr, however with Mr Ponosh’s advice, these is a very infrequent and rare outcome.
Content coming soon…
Content coming soon…
Pelvic venous congestion syndrome (PVCS) is a cause of chronic pelvic pain and is a secondary cause of leg varicose veins in approximately 13-40% of women. Pelvic congestion syndrome is condition often caused by the dilatation of the ovarian or other pelvic veins, like varicose veins but in the pelvis.
However, in almost all cases, the treatment of PVCS is very simple.
Varicose veins are most commonly seen in the legs. They occur due to a failure of the valves in the leg veins (see Varicose Vein Information sheet for more details). This causes the blood to pool, causing enlarged, bulging and dilated veins. This is also what happens to the pelvic veins in PVCS. This pressure can cause a number of abdominal or pelvic complaints but can also be a cause of lower limb varicose veins and swelling, through the indirect pressurization of leg veins.
In men, PCVS through the malfunctioning of a testicular or gonadal vein (the male equivalent of the ovarian vein), can cause dilated veins in the testicles (varicocele), testicular discomfort, infertility and varicose veins. This is treated in a similar fashion to PCVS.
Another associated condition is May-Thurner Syndrome. This condition can cause PCVS but can more commonly cause left leg swelling and can be a cause of deep vein thrombosis (DVT). This is caused by compression of your left iliac veins by your iliac arteries causing blood to pool in your leg. Whilst a minimal degree of compression is present in all of us, in rare cases the compression is severe and needs treatment.
The cause of the dilated ovarian/pelvic veins in PVCS is poorly understood. PVCS most commonly occurs in who have had children. During pregnancy the ovarian vein can be compressed by the enlarging womb or enlarged because of the increased blood flow. This is thought to affect the valves in the vein causing them to stop working. This causes poor pelvic drainage and pooling of blood in the pelvic veins.
There are other causes that may cause obstruction to the ovarian and pelvic veins leading to PVCS, which are much less common. It can also occur spontaneously or associated with an aberrant venous anatomy. PVCS may also be associated with polycystic ovaries. The absence of the vein valves due abnormal development may also be a contributing factor.
The varicose veins in the pelvis surround the ovary and can also push on the bladder and rectum. This can cause the following symptoms:
Your GP may suspect PCVS or you may be asked to see Mr Ponosh in regards to your abdominal symptoms or leg varicose veins. Your GP may contact Mr Ponosh’s office directly, however in some cases they will provide you a referral to contact the office yourself. Mr Ponosh’s caring and helpful staff will walk you through the process of making an appointment with Mr Ponosh. His staff may also contact you directly. For further information regarding referrals, please go to Make an Appointment.
When you see Mr Ponosh, he will undertake a full history and appropriate examination. In cases of PCVS, the diagnosis is mainly based upon your history, symptoms and examination – this is critical. In many instances he will order appropriate tests before he sees you to streamline your management and avoid unnecessary appointments. These tests are bulk-billed. The most common tests to assist the diagnosis of PCVS may be a specialized abdominal and leg vascular ultrasound and in some cases a CT scan. In very rare cases a MRI scan may be arranged but normally only after seeing Mr Ponosh.
Based upon Mr Ponosh’s expert specialized review, an appropriate treatment plan will be suggested and explained to you in an open, straight-forward, jargon-free manner with all options and questions addressed.
Pain can be a common symptom and present for over 6 months duration. The pain is usually on one side but can affect both sides. The pain is worse on standing, lifting, when you are tired, during pregnancy and during or after sexual intercourse. The veins are also affected by the menstrual cycle/hormones and therefore the pain can increase during the time of menstruation. The pain usually is improved by lying down.
PCVS is a significant and common cause of complicated and unusual leg vein issues
Although ultrasound, CT and MRI may be initially used, PCVS is notoriously difficult to diagnose on imaging and in many cases is not clearly defined. This is not a failure of the test but is a reflection of the challenging and difficult assessment of the presence and function of these veins.
Even if the imaging does not clearly show evidence of PCVS, if Mr Ponosh suspects its presence from his vast clinical experience he may recommend an Abdominal Venogram.
This is a low risk, minimally invasive procedure usually conducted as a day case in hospital under local anaesthetic and light sedation so is essentially pain free (please refer to Angiogram & Venogram Information). In a specialized x-ray room, a small needle is placed in your groin and under x-ray guided imaging and through the injection of contrast dye, the nature of your abdominal veins and any evidence of PCVS is identified. This may appear as varicose veins in your pelvis, dilated ovarian or pelvic veins or in some cases compression of other draining veins. You will be asked to hold your breath several times and occasionally a special CT scan may be taken during your procedure (Dyna CT) for very detailed assessment.
If PCVS is confirmed, usually through the identification of a dilated ovarian vein, Mr Ponosh will proceed to definitively treat this during the same procedure. The malfunctioning vein (usually the left but in some cases the right or both) is entered with a fine wire and tube (1mm in size) and the vein is permanently blocked off with tiny coils which cause the vein to block off in a controlled and planned fashion. This is known as “coil embolization”. The treatment of these dilated veins stops the blood pooling in the pelvis and stops the venous congestion and hypertension that causes your symptoms.
The venogram takes approximately 20 minutes and if found the “coil embolization” takes an additional 10 minutes. The benefit of this procedure is that it is definitive. It is the only way of without doubt confirming or excluding PCVS and treating it in the same procedure. In rare instances where PCVS is not found, this is still of significant clinical benefit as it excludes the condition without a doubt. If it is present, it is easily treated. Apart from being extremely low risk and minimally invasive, it has a rapid recovery.
In cases of May-Thurner Syndrome, a venogram is also undertaken but if found, it is usually treated with a balloon venoplasty (stretching the vein) or placing a stent to permanently treat the narrowing. Mr Ponosh will discuss this further with you if suspected. Please see Angiogram & Venogram Information for further details.
Mr Ponosh is a no gap provider so there is no cost for this procedure for all private health funds
Following the procedure, some gentle pressure is applied to your groin. You rest in bed for approximately 3 hours and you in almost all instances are home later in the day. Mr Ponosh recommends a quiet day or two at home but the procedure has little impact on your day to day life.
Pain following the procedure is usually minimal. A dull ache in the groin is not uncommon and well controlled with paracetamol. Following the procedure, bed rest is required for a short time and most people leave the hospital within 4 hours of the procedure.
Once discharged, you are able to resume your normal activities within the first 24-48 hours. The best advice is not to over exert yourself and avoid heavy lifting or strenuous gym work for 5-7 days.
Some people may develop an aching back or loin pain, similar to period pain for a few days following the procedure as the embolized veins completely block off. This resolves rapidly and is well controlled with regular oral pain medications.
By treating your PCVS , the pelvic varicose veins should gradually shrink away over a few weeks and your symptoms improve. As the main ovarian and pelvic veins have been embolised, if you also have any lower leg varices, these can now be treated with a reduced chance of them coming back in the future (which they have a high chance of coming back if you did not have the pelvic vein embolisation). Mr Ponosh will discuss your leg vein management in detail with you. Any symptoms that you have been having related to the varicose veins in the pelvis should also slowly improve.